This post is also available in: Português (Portuguese (Brazil))
The use of stimulant drugs is growing in different parts of the world. In 2018, the World Drug Report showed that amphetamine-type substances (ATS) are the second most commonly used illicit drug – after cannabis – with an estimated 34.2 million past-year users. ATS is mostly used in North America and Oceania, but its use has sharply increased in many countries in East and South-East Asia. Cocaine had an estimate of 18.2 million past-year users worldwide, and its use is also rising in some parts of the world, such as Europe. In Latin America, North America and the Caribbean, cocaine has had a long-lasting presence, and it is still the primary drug of concern, after cannabis. Besides, many of the New Psychoactive Substances are synthetic stimulants.
Literature review
A review of the literature on effective harm reduction interventions for people who use stimulants
Description of good practices
The description of seven cases of good harm reduction practices for people who use stimulants in different world regions


Safer smoking kits, for instance, help people to increase safe-smoking practices; decrease injection; decrease/cease use of home-made pipes; reduce burns to mouth and throat; reduce damage to lungs.

Using cannabis (plant-based substitution) helps some people to diminish anxiety, aggression, and paranoia for crack use. It also helps them reduce craving, stimulate appetite and promote sleep.

To enhance self-regulation strategies allows people to be aware and increasingly use their own self-care strategies. It also helps to deal with emotions without recurring to problematic drug use.

Drug Consumption Rooms help people to have a safe, non-rushed environment; access sterile equipment (such as safer smoking kits|); access care services; prevent overdoses, enhance safer drug use practices, and prevent transmission of infectious diseases.

Simple therapeutic interventions (mental health-related) can help people who use stimulants suffering from paranoid thoughts, anxiety, hallucinations or withdrawal. They also help to identify problems and commit to change and to create a support network and manage drug use.

To offer people a safe place to be during the day in drop-in centers help them to improve wellbeing, (mental) health, social engagement, reduce drug use and reduce the exchange of sex for drugs.

Providing people with housing (housing first) reduces their exposure to drug use; decrease use; increases treatment adherence and autonomy; helps to develop healthier sleep/eating patterns.
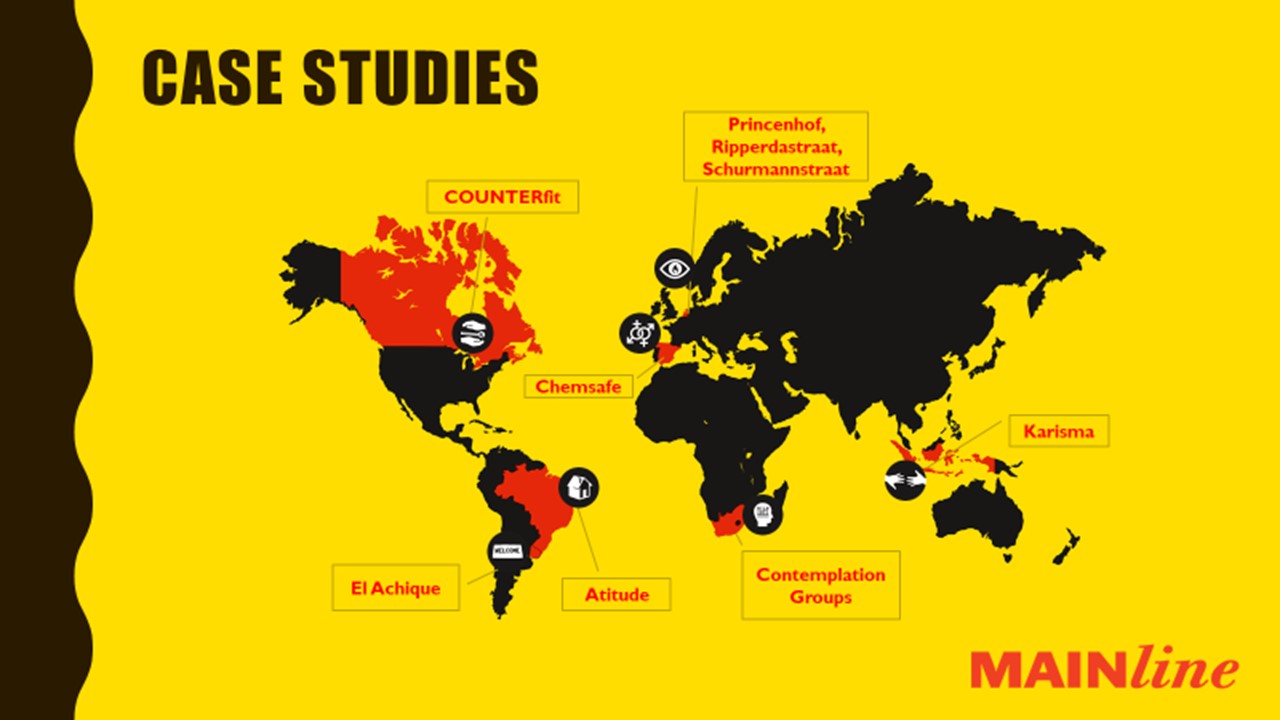
Atitude
Offering housing first, drop-in centers, shelter, and outreach work for people using crack cocaine in Brazil;
Contemplation groups
Enhancing self-regulation strategies for people using methamphetamine in South Africa;
Drug Consumption Rooms
Assisting people using crack cocaine in the Netherlands;
Karisma
Offering outreach work for people using methamphetamine in Indonesia;
El Achique
A drop-in center for people using cocaine base paste in Uruguay;
COUNTERfit
A multi-service program distributing safer smoking kits for people using methamphetamine and/or freebase cocaine in Canada, and
Chem-Safe
An online intervention for people using stimulants while practicing chemsex in Spain.
Do we need specific harm reduction for stimulants?
*Technical facts (or who are "we"):
Research team: Rafaela Rigoni (me, as a lead researcher), Joost Breeksema & Sara Woods.
Organization: Mainline
Period: September 2017 – June 2018Funder: GPDPD (Global Partnership for Drug Policy and Development) program, implemented by GIZ on behalf of the German Federal Ministry for Economic Cooperation and Development.








